
Welcome to this video on newborn Apgar score! The newborn Apgar scoring system was designed by Dr. Virginia Apgar in 1952 to evaluate the physical condition of the newborn at birth and the immediate need for resuscitation.
Apgar Criteria
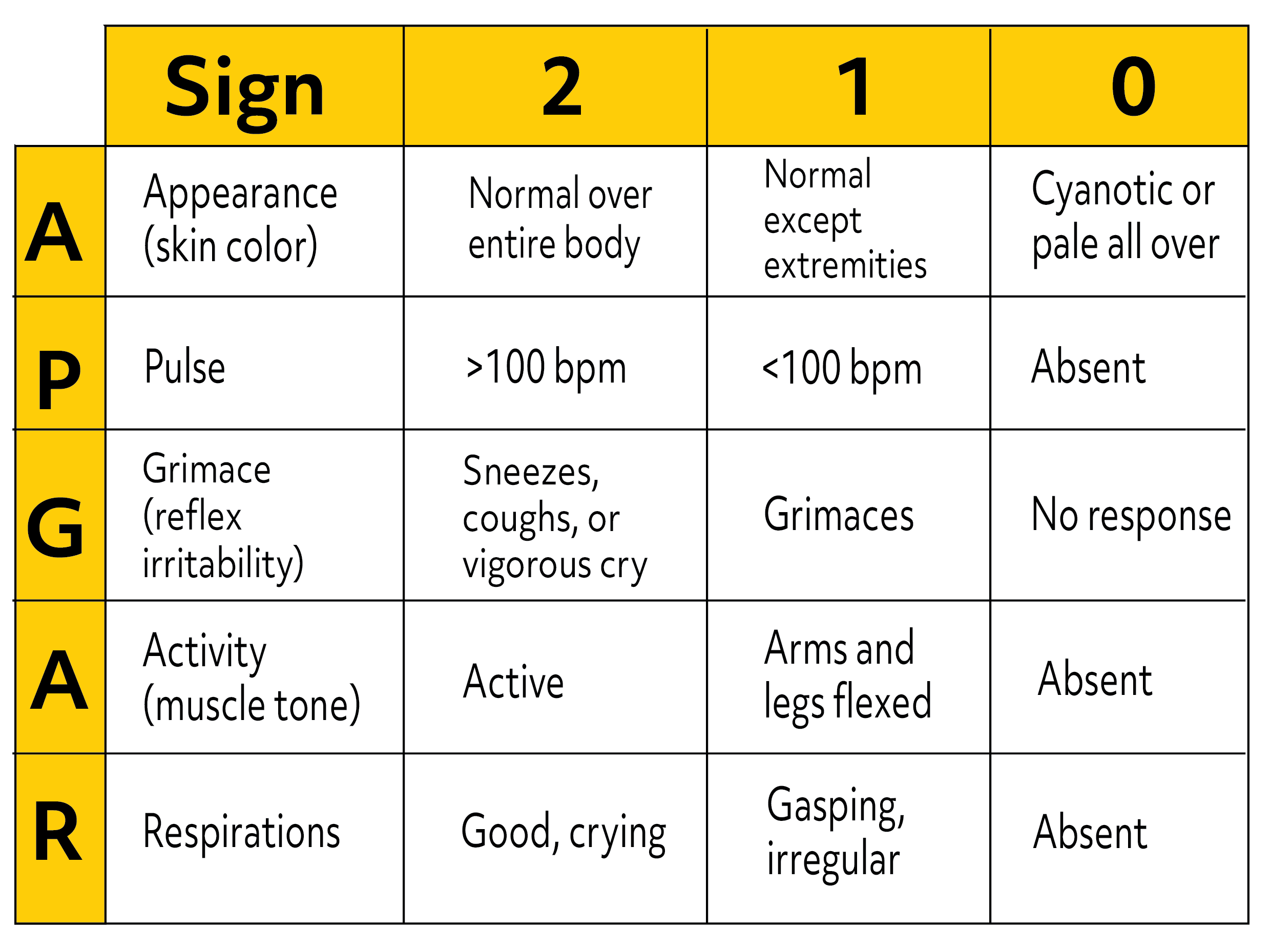
The newborn is rated on 5 different criteria, each scored from 0 to 2, for a total scoring range from 0 to 10. The newborn is rated 1 minute after birth and again at 5 minutes on the following criteria:
A – Appearance
Skin color is inspected for cyanosis and pallor. 85% of normal newborns have blue extremities with the rest of the body pink at 1 minute after birth, which is called acrocyanosis and rates a score of 1. An infant that is blue or pale all over scores 0, and a completely pink newborn scores a 2.
P – Pulse
The pulse is palpated or auscultated at the junction of the umbilical cord and skin and is a turning point assessment. A heart rate less than 100 beats per minute indicates the need for immediate resuscitation. If the pulse rate is absent, score is 0. Pulse less than 100 beats per minute, scores 1, and pulse greater than 100 beats per minute, scores a 2.
G – Grimace
Grimace, or reflex irritability, can be evaluated by stroking the soles of an infant’s feet. No response to stimulation scores 0, a grimace from aggressive stimulation scores 1, and a cough, sneeze, or vigorous cry receives a score of 2.
A – Activity
The activity, or muscle tone, is determined by evaluating the degree of flexion and resistance to straightening of the extremities. A normal newborn’s elbows and hips are flexed, with the knees positioned up toward the abdomen. If the baby is limp, the score is 0, some flexion scores a 1, and active motion scores 2.
R – Respiration
Respiratory effort is a very important Apgar assessment. Complete absence of respirations is called apnea, and scores 0. Gasping or weak respiratory effort scores 1, and a vigorous cry indicates good respirations, scoring a 2.
If the infant receives a score less than 7 at the 5-minute interval, then scoring continues at 5-minute intervals thereafter up to 20 minutes. The Neonatal Resuscitation Program guidelines state that the Apgar score is “…useful for conveying information about the newborn’s overall status and response to resuscitation. However, resuscitation must be initiated before the 1-minute score is assigned. Therefore, the Apgar score is not used to determine the need for initial resuscitation, what resuscitation steps are necessary, or when to use them.” If an Apgar score remains 0 beyond 10 minutes of age, discontinuation of resuscitative efforts may be appropriate.
Apgar Score Results
When the 5-minute Apgar score of a term and late-preterm infant is 7-10, it is defined as reassuring, a score of 4-6 is moderately abnormal, and a score of 0-3 is low. When the 1-minute Apgar score is 0-3, it is not a prediction of any individual infant’s outcome; however, a score of 0-3 at 5 minutes is consistent with neonatal mortality, but does not predict future neurologic dysfunction. The Apgar score expresses the infant’s physiologic condition immediately after birth and the infant’s response to resuscitation if needed. Remember the 5 components scored include: color, heart rate, reflexes, muscle tone, and respiration.
Review Questions
Let’s go over a couple of questions for review:
The nurse is assessing a newborn 1 minute after birth, and she notes acrocyanosis, heart rate of 118 bpm, legs withdraw with foot stimulation, active motion, and a weak cry. The 1-minute Apgar score for this infant would be
- 7
- 8
- 9
- 10
The acrocyanosis, or blue extremities, and a weak cry, each receive a score of 1, reflecting a total score of 8.
Let’s try another one – An infant receives an Apgar score of 4 at 1-minute and 6 at the 5-minute interval. What should happen next, regarding Apgar scoring?
- Apgar scoring is complete, 4 and 6 are adequate scores.
- Another Apgar score should be done at the next 5-minute interval
- Apgar scoring should continue every 5 minutes, until the score is 7 or above, or 20 minutes is reached.
- Answer B & C are correct
If the infant receives a score less than 7 at the 5 minute interval, then scoring continues at 5-minute intervals thereafter up to 20 minutes.
Thank you for watching this video review about the newborn Apgar score – I hope it helps your studying!

